Turn up the AC ... what is going on with this Southern Surge?
- Jeffrey Morris

- Jun 24, 2020
- 10 min read
Since states started opening up from stay-at-home orders in late April, we have seen heterogeneous results. Some states have showed continuing declines after opening, while others seem to be in a plateau steady-state of infections that are not decreasing but not showing signs of increase either, while some states have experienced upticks in the past several weeks that have transformed into alarming and undeniable surges, most notably, Arizona, Texas, Florida and South Carolina.
I have been racking my brain trying to understand what has been going on in these locations -- why have surges happened in these locations and not others? Why are they happening now and not sooner? I've seen narratives floated in the media suggesting this is inevitable after reopening, but that doesn't make sense to me as I've seen numerous areas with no evidence of problems yet after reopening, and of these four locations, only Arizona showed immediate uptick after reopening -- the others seemed stable for several weeks after reopening and then at some point experienced a notable surge. Let's look at the incidence curves for these states to see some of the data, and then I'll try to describe what I think are the key factors contributing to this southern surge.
Texas
Here is the daily incidence curve for TX over time from our web app, showing new cases per day, smoothed using a 7-day moving average to remove day-to-day noise and day-of-week effects.

Texas opened on 4/30, and remained relatively steady through the end of May, even with increasing testing. However, starting about May 27, we see an increasing trend that appears to have accelerated as of about June 14, a sharp increase that continues now during this surge. The magnitude of this surge is far beyond what can be explained by any increase in testing.
Some of the early increases were driven by Dallas and Houston, but recently has expanded into other areas of Texas including San Antonio and Austin areas. I've followed Houston closely, so let's look at these numbers assembled for the greater Houston area on the Texas Medical Center website. Here is the increase in cases:

We see the similar pattern in Houston metro numbers in new cases/day, with an uptick evident at the end of May and early June, but sharply accelerating in mid-June at an alarming rate, with the cases/day doubling or tripling in the past week. If this continues things could get out of hand very very quickly.
Look at the hospitalization numbers from the TMC:

I have been watching these very closely, as any true surge in infections will likely be accompanied by an increase in hospitalizations. We also see a steady increase in new covid-19 related daily hospitalizations starting late May, and again sharply accelerating in the past week or two. The number of new hospitalizations has doubled in the past 10 days, and tripled in the month of June. This is also alarming, and recall that hospitalizations are lagged behind cases, so it is likely the hospital surge expected to accompany the increase in cases since 6/14 is not reflected in the data yet. There are reports that the ICUs in Houston are reaching capacity (97% of normal capacity according to friend David Hong, and about to start moving into surge capacity) and patients are having to be moved to other hospitals, even clearing out space in Texas Children's Hospital to take on some adult COVID-19 patients.
Florida
Like Texas, Florida seemed to be doing OK after reopening in early May, with flat daily cases along with a doubling in daily testing rates throughout the month of May. But then on June 1st, a clear uptick started, and the slope has sharply increased since June 14th or so, far outpacing any increase in testing, and indicating an undeniable surge:

Here is the incidence table from Tallahassee Reports:

The state opened most counties on May 4, but held out Miami-Dade and Broward counties that showed upticks in May until May 18th, which is what is meant by "Phase 1 Full Reopening". They are certainly in midst of a full-blown surge. Here are the daily new covid-19 hospitalizations according to the same site:

The surge in cases has not yet produced any increase in daily new covid-19 related hospitalizations, but since hospitalizations are lagged behind cases, it is possible that given the surge in cases is so recent the corresponding hospitalizations have not occurred yet -- this bears watching.
South Carolina
Here is the incidence curve showing the 7-day moving average of new daily cases for South Carolina.

Once again, we see an uptick starting at the end of May, followed by an accelerated increase, here starting about June 7th or so. Here is the corresponding data from the South Carolina website:

Unlike other states, South Carolina has not shown an uptick in testing, so it is possible that these numbers underrepresent the magnitude of the surge as well. The high test positivity rate (proportion of SARS-CoV-2 molecular tests that are positive) suggests a lower testing rate than most other states, and the increasing test positivity rate suggests a true surge in infections:

Arizona
Here is the incidence curve for Arizona, the 7-day moving average of daily new covid-19 cases:

Arizona reopened on May 15th, and showed clear evidence of an uptick within two weeks of opening, and then a sharp acceleration in the growth rate about two weeks later, again around June 14th. This increase has the highest slope of any state in the nation, and is staggering and alarming. By far the worst hit area in the state is the Phoenix area (Maricopa county). Here is the daily new case count for this county from the Maricopa county website:
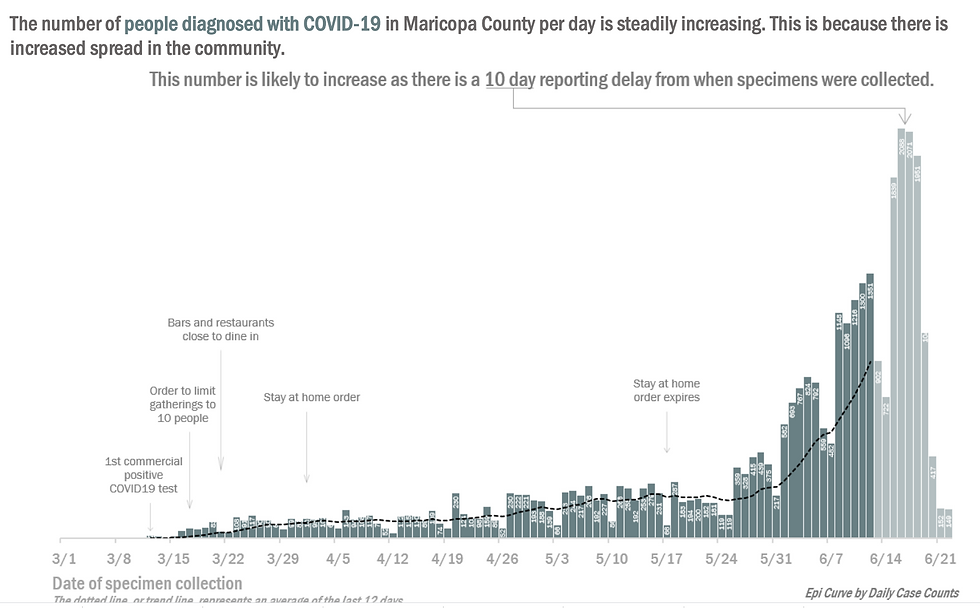
This is the most staggering graph I have seen in the USA during this entire pandemic. The daily case rates are now rivaling Queen, NY's during the peak of their surge, and is accelerating at an alarming rate. Note that the data from 6/14 until present are greyed out, indicating those counts are still not complete and will likely rise given they date a case on date specimen obtained and some tests on those days are still pending. Here are the corresponding hospitalization numbers:
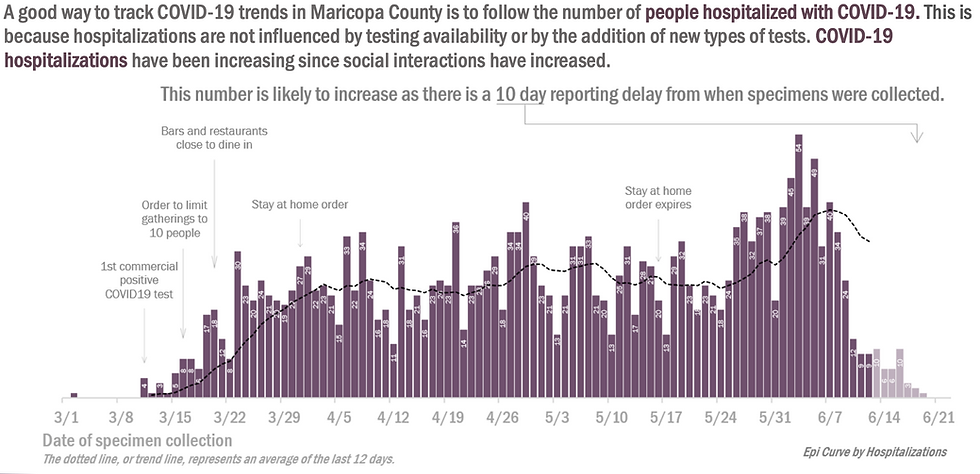
We see the hospitalization numbers show nearly a doubling from 5/17 until 6/1 or so. Since hospitalizations are lagged further behind cases and since they date a hospitalization on the date specimens are collected, it is likely these data do not yet reflect the accelerated surge in the past two weeks that have tripled the number of daily cases. There are already reports of Arizona hospitals becoming overwhelmed, and if there is a growth in hospitalizations proportional to the growth in cases of the past two weeks, it could be a very dangerous setting.
Factors driving this surge
So why are these states experiencing these surges, and other states that opened have not? And for some of these states, why the delayed surges and sharp acceleration in June? These are key questions to understand, both to help these states manage their crisis as well as to prevent similar surges from occurring elsewhere. There could be several factors at work that I will mention in what I consider to be decreasing levels of importance:
Insufficient vigilance
Critical mass of disease
Summer tourism
Shift Indoors to AC
Insufficient vigilance: After reopening, CDC and other community guidelines recommend certain precautionary steps be taken to limit the chance of a resurgence. This includes maintaining social distancing measures, especially avoiding big crowds indoors in enclosed spaces that are ideal for viral spread, and mask-wearing, especially when indoors and around other people. Unfortunately, I have not been able to find any reliable source of information on mask-wearing, but from discussions with people in these states, and in particular in the urban and coastal areas in which the surge is most evident, mask-wearing has been rare in these locations. This may be related to cultural or political attitudes, as I have heard people in these areas equating mask wearing with weakness or having doubts about whether the viral threat is real or way overblown by media or politically motivated hype. In terms of social distancing, the capacity and distancing recommendations might not be followed or enforced rigorously enough, and crowded, indoor locations with inadequate distancing and a lack of mask wearing is a recipe for rapid spread. Also, there is strong evidence that this southern surge has a much higher proportion of young adults, 20's and 30's, than previous reported infections, and it may be this age group that is letting their guard down and engaging in potentially risky behavior at a higher clip. Unacast uses cell phone data to track certain social distancing measure -- in our modeling we have found the visits to nonessential businesses to be the most predictive measure of spread risk. During lockdowns, this measure decreased to 70-75% below pre-covid levels, and has crept up to roughly 30% below pre-covid levels in many places (see solid lines in plots below for national average). These may suggest people are going out too much, too quickly -- South Carolina shows almost full return to pre-covid levels, and if you look at coastal counties these numbers are more extreme. These could be showing that some people are doing too much or too quickly. And not included in the data is whether social distancing or mask wearing is being practiced at these non-essential businesses -- in areas where people are not taking the viral risk as seriously, they may not be practicing the recommended distancing and mask wearing that would make the visits to non-essential businesses safe.
Texas:

Florida:
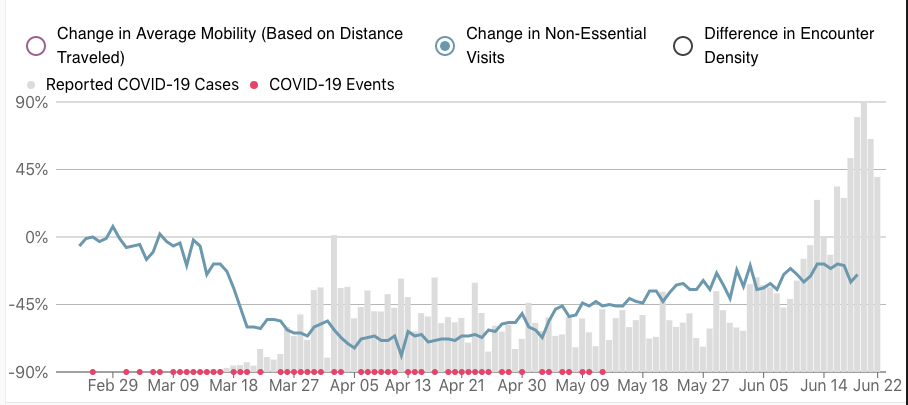
South Carolina:

Arizona:

Critical Mass of Disease: In areas of high population density, it is possible for an uptick to very quickly turn into a surge because of the high numbers of infected and sheer numbers of susceptible people they encounter. Thus, a sustained uptick in cases in urban areas can quickly become a surge if the proper precautions are not being taken. Although the uptick in cases is evident more broadly, we have seen in Texas, Arizona, and Florida, the surges are most evident in the densely populated urban areas. We have to be extra careful in these areas to monitor upticks before they get out of control since they are much more difficult to reign in because of their dense environments, plus there are a lot more opportunities for spread into neighboring communities.
Summer Tourism: The upticks in Florida, South Carolina, and some parts of Texas seem to have started about 2 weeks after Memorial Day weekend, and the social distancing measures in coastal counties in South Carolina and Florida suggest tourism is providing a major increase in population density and person-to-person interactions in these locations, contributing to increased spread especially when accompanied by lax distancing practices in restaurants and bars and minimal mask-wearing. It seems likely that this factor is not primarily driven by beaches and other outdoor activities, but indoor activities that vacationers tend to participate in the evenings. We have seen numerous reports and papers showing how much more efficiently the virus spreads indoors than outdoors, and the lack of any evidence of surges two weeks after BLM-inspired protests in various cities across the country, which were almost exclusively outdoor events, supports this notion. This leads me to the last factor.
Shift Indoors to AC: What is one thing that these 4 states experiencing June surges share? They all have become too hot to comfortably participate in outdoor activities. The average high temperature in Phoenix is >100 degrees in June, in Houston the heat and humidity kicks in during the month of June, and Florida and South Carolina also transition to a much less comfortable hot and humid weather in June than in April and May. As people flock to air-conditioned settings, indoors with recirculated air, that could be a contributing factor to these upticks and surges. In the Northeast, the June weather is very pleasant, and individuals are engaging in more outdoor activities than earlier in the Spring, and so may be experiencing protection against infection relative to the south where it has become unbearable to be outside for long periods of time. Our modeling results and numerous publications have clearly shown that increasing temperatures and humidity reduce the efficiency of spread of a respiratory virus like SARS-CoV-2, but once people start spending more time indoors, that may counteract this effect.
Conclusions:
It seems a perfect storm has been brewing in these southern states, with lockdown fatigue releasing a pent-up demand for people to get out and about, lack of vigilance in businesses to enforce social distancing guidelines, a individualistic culture resistant to mask wearing, dense populations with increasing tourism leading to even greater crowding, and shifts in weather leading people to spend more time indoors. Now that these upticks have produced case numbers in the hundreds and thousands, there is critical mass for the resumption of exponential growth that is apparent in these four states.
So what can be done about it? Parts of Arizona, Texas, and Florida have instituted mask-wearing directives, and this will help and needs to be expanded, and public compliance with these directives is needed -- mask wearing may be unnecessary outdoors or when not near others indoors, but indoors when around other people, especially in crowded areas, they can make a huge difference. Mask wearing is not an issue of politics or freedom, it is an issue of public health in this pandemic, and it is a LACK of mask wearing that will lead to a loss of freedom if surges happen that lead to further lockdowns.
Additionally, businesses such as restaurants and bars need to follow the capacity restrictions in place. Some places may be tempted to let them slide, but these environments can be the most susceptible to super spread events, and so it is in their best financial interest to prevent these events.
These steps may not be enough to step the tide in places where the surge is accelerating so quickly, so the communities most affected by this surge may also need to consider rolling back some aspects of the reopening. From this blog my viewpoints on lockdowns are well documented: Because of the extensive collateral damage they impose on society, they are not sustainable long term and should be replaced by targeted mitigation strategies that can be sustained over time. That we should identify the key precautionary steps we can take that maximize the reduction of viral spread while enabling people to live as much of a normal life as possible. But if these precautionary steps are not followed, then surges like this one in the south may result that require more extreme mitigation measures to get under control. If this is necessary, my hope is that officials can identify which aspects of the reopening are causing the most risk and only roll those back -- to not reflexively try to go back to stay-at-home orders. And once under control, I hope we can find and follow the targeted steps to prevent them from happening again.
This message is also important for other locations with similar factors, including southern states like Georgia, North Carolina, Alabama, Mississippi, Louisiana, Arkansas, Oklahoma and Tennessee as well as western states including Utah, Nevada, and desert California. These places may be prone to this same surge, and many have shown some evidence of upticks in the past few weeks, so need to be vigilant to take the steps to avoid joining the surge currently experienced in these four states. Their proximity to Arizona, Texas, Florida and South Carolina, very highly populated states, may contribute to the potential for a surge given the increased interstate travel that has picked up in the past month.
Comments on Death Rates:
Some people look at the decreasing COVID-19 related death rates, and think this means we should not be concerned about this surge in cases. There are a number of factors related to this, but breaking these down requires an involved discussion that I am saving for a future blog post later this week. Suffice it to say that I think it would be very unwise to let this cause us to downplay the risk of the current surge.



Valuable content and presentation <->} Crown Town Pune {} Ravet Crown {} Nigdi Crown {} Wakad Crown {} Marunji Crown {} Hinjewadi Crown {} Pcmc Crown {} Baner Crown {} Aundh Crown {} Pimple Saudagar Crown {] Shivaji Nagar Crown {] Kalyani Nagar Crown {} Viman Nagar Crown {} Koregaon Park Crown {} Kharadi Crown {} Magarpatta city Crown {] Deccan Crown }{ {] Bavdhan Crown
it’s an absolute must-read ! Link.. I appreciate you sharing such thoughtful content. LINK
Aundh Link
Hinjewadi Link
Wakad Link
Baner Link
Ravet Link
Balewadi Link
Pimple Saudagar Link
Shivaji Nagar Link
Koregaon Park Link
Viman Nagar Link
Magarpatta Link
Bavdhan Link
Main Pune Link
Kothrud Link
Pimpri-Chinchwad Link
Best In Pune
The Real Pune Service I chose possessed a remarkable combination of charm, intellect, and beauty. From start to finish, the service was flawless, and I felt completely at ease the entire time.
Ukraine is currently at war and thousands of innocent people are dying, who simply lived in their own country and did their usual things. Russia has declared war on Ukraine and is killing civilians. To read true information or help Ukraine go to the site.